MeNZB Immunisation Programme effectiveness shown
8 August 2006
Media Release
Meningococcal B Immunisation Programme effectiveness shown
Children and young New Zealanders who are not immunised against the epidemic strain of group B Meningococcal disease have a five times higher risk of getting it than those who are fully-immunised, preliminary results from an independent study show.
Dr Richard Arnold, head of the Victoria University team which carried out the effectiveness study, said the staggered roll-out of the MeNZB(TM) immunisation programme meant their statistical model could separate the effects of the vaccine from the effects of the natural progression of the epidemic over time.
"Our results show there is a five-fold reduction in disease rates among fully vaccinated New Zealanders, "says Dr Arnold. The data are yet to be finalised and will be published in a scientific peer-reviewed journal later this year.
Melbourne University Professor Terry Nolan, chairperson of the Vaccine Effectiveness Peer Review Group, says the methods that have been used to assess the effect of the vaccine on meningococcal disease are robust and are in line with best practice used to evaluate other vaccines.
The staggered roll-out meant it was not until mid-2005 that a significant number of New Zealanders were fully immunised, but the initial impact of the vaccine has seen a critical reduction in the number of epidemic strain Meningococcal B cases since the immunisation programme began.
In the northern region, where the programme started, cases of the epidemic strain fell by 76 per cent between 2003 and 2005. In Maori and Pacific communities, with the highest rates of the disease, cases fell by 90 per cent and 70 per cent respectively.
Meningococcal B Immunisation Programme Director Dr Jane O'Hallahan says if current trends continue, we will have made substantial progress towards ending the epidemic by the end of the year - several years earlier than it would have taken to end naturally.
Since the start of the epidemic in 1991, there have been more than 5900 cases and 239 deaths from meningococcal disease. An estimated 20 per cent of sufferers are left with some degree of disability including hearing loss, brain damage, and amputation or scarring.
The Government committed $200 million to the Meningococcal Vaccine Strategy which has paid for the development of a strain-specific vaccine, clinical trials and implementation of our biggest mass immunisation campaign for all New Zealanders under 20 years old, and has announced a further $22 million over the next three years to extend the programme.
The programme, coupled with the excellent vaccine uptake, has helped drastically reduce the number of children afflicted by this disease, however it is important for those who are not fully immunised to make sure they complete their vaccinations, Dr O'Hallahan says.
"The effectiveness study confirms that the vaccine works. It is important that children and young people complete all three doses. For young babies who began their vaccinations before they were six months old, it is critical that they have all four doses."
Under-20s will now have until the end of the year to complete all three doses, while newborns and under-fives will continue to be offered the programme until 2009, or until disease rates indicate we can end the programme sooner, Dr O'Hallahan says.
It is important to remember that no vaccine provides 100 per cent protection. Most people who are immunised with MeNZBâ„¢ vaccine are protected, but the vaccine may not protect every person who receives the full course. The MeNZBâ„¢ vaccine will not protect against other strains of meningococcal disease so people need to be vigilant about the signs and symptoms of the disease.
Effectiveness data has been analysed by the Victoria University team and the methodology peer-reviewed by an independent group led by Professor Nolan.There is considerable international interest in the findings.
The success of the immunisation programme is due to the efforts of many people, including Novartis Vaccines whose scientists worked to develop and manufacture the vaccine on an accelerated timetable to support the New Zealand programme, the University of Auckland team led by Professor Diana Lennon, Institute of Environmental Science and Research staff led by Dr Diana Martin, District Health Boards, GPs, practice nurses and practice managers, public health nurses, Maori and Pacific Island providers, Ministry of Health staff and a huge number of others.
--
For further information on the reduction in epidemic strain Meningococcal B cases please see the attached graphs
See...
Cumulative numbers of epidemic strain
meningococcal disease cases in the Northern Region among
individuals aged 6 weeks to 19 years 2002-2006
(PDF)
Cumulative numbers of epidemic strain
meningococcal disease cases in New Zealand excluding
Northern Region in individuals aged 6 weeks to 19 year olds
2002 - 2006 (PDF)
Image versions:
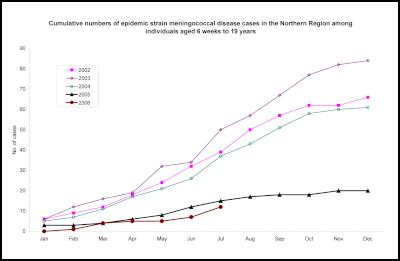
Click to enlarge
Cumulative numbers of epidemic strain meningococcal disease cases in the Northern Region among individuals aged 6 weeks to 19 years
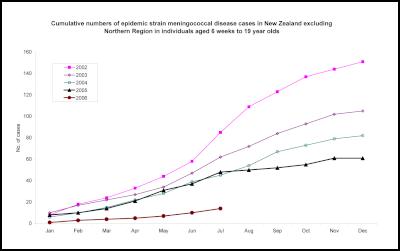
Click to enlarge
Cumulative numbers of epidemic strain meningococcal disease cases in New Zealand excluding Northern Region in individuals aged 6 weeks to 19 year olds
QUESTIONS AND ANSWERS
What is
meningococcal disease?
Meningococcal disease is a
bacterial infection. It causes severe illnesses including
meningitis (an infection of membranes that cover the brain)
and septicaemia (a serious infection in the blood). There
are several strains of bacteria which cause meningococcal
disease including A, B and C. MeNZBâ„¢vaccine was developed
to protect against the strain of meningococcal B causing the
New Zealand epidemic. Everybody in New Zealand is at risk of
contracting the disease, however about half of epidemic
strain cases in New Zealanders under 20 years old were in
children aged under five years. Meningococcal disease rates
for Mäori and Pacific peoples are particularly high.
What proportion of New Zealanders in the eligible age
group have received the MeNZBâ„¢vaccine?
As at 2 July
2006, 87 per cent of all those eligible for the vaccine had
completed their first dose, with 80 per cent having
completed all three doses.
Does the MeNZBâ„¢vaccine work?
Yes. Preliminary results from the study confirm that the
vaccine is 80 per cent effective.
In the five years
before the introduction of the vaccine there was an average
of 213 cases and seven deaths per year in under 20 year olds
from the epidemic strain. In 2005 there were 82 epidemic
strain cases and one death in this age group and in the
seven months of 2006 there have been 23 cases and no deaths.
The vaccine will continue providing protection year after
year for the natural course of the epidemic.
When is the
MeNZBâ„¢ vaccine given?
It is recommended that babies
begin their MeNZBâ„¢ vaccinations at six weeks of age,
followed by a second dose at 13 weeks or three months, a
third dose at 21 weeks or five months and a fourth dose at
43 weeks or 10 months. For all other ages, three doses
should be given at six-weekly intervals.
Is the
MeNZBâ„¢vaccine safe?
Yes.There are no live
meningococcal bacteria in MeNZBâ„¢ vaccine and it is not
possible to catch the disease, or to become a carrier of the
disease, from the vaccine. The vaccine has been manufactured
to international standards. Extensive safety data collected
during the programme was reviewed by an Independent Safety
Monitoring Board (ISMB). The ISMB has stated that based on
the data it has seen, it has no concerns regarding the
safety of the MeNZBâ„¢ vaccine. Serious side effects are
very rare however some people experience a mild temporary
reaction such as redness at the site of the injection, a
headache, nausea, a slight fever, feeling unwell, drowsy or
irritable.
If I am immunised can I still get
meningococcal disease?
No vaccine provides 100 per cent
protection. Most people who are immunised with MeNZBâ„¢
vaccine are protected against the epidemic strain, but the
vaccine may not protect every person who receives the full
course. The MeNZBâ„¢ vaccine will not protect against other
strains of meningococcal disease and there is also up to a
28-day delay after the full course is completed for
immunity to develop. People still need to be vigilant about
the signs and symptoms of the disease. In the early stages
the disease may look like influenza. It can progress very
quickly and is difficult to diagnose. A baby or child might
have a fever, be crying or unsettled, refuse drinks or
feeds, vomit, be sleepy, floppy or hard to wake, dislike
bright lights or have a rash or spots. An adult may have a
fever or headache, a stiff neck, joint pain and aching
muscles, vomit, be sleepy, confused, delirious or
unconscious, dislike bright lights, have a rash or spots.
If you are concerned that you or someone in your household
has meningococcal disease, ring a doctor or medical centre
urgently.
ENDS


 Race Unity Speech Awards: Students’ Vision For A United Future - Embrace Our Differences
Race Unity Speech Awards: Students’ Vision For A United Future - Embrace Our Differences Commonwealth Foundation: Commonwealth Short Story Prize 2026 Regional Winners Announced
Commonwealth Foundation: Commonwealth Short Story Prize 2026 Regional Winners Announced Doc Edge Festival: World Press Photo And Doc Edge Comes To Auckland In Landmark Exhibition Merger
Doc Edge Festival: World Press Photo And Doc Edge Comes To Auckland In Landmark Exhibition Merger Whakarongorau Aotearoa: International Nurses Day - Healthline Nurses Help 800 New Zealanders A Day
Whakarongorau Aotearoa: International Nurses Day - Healthline Nurses Help 800 New Zealanders A Day NZ Psychological Society: Remembering The Past Guides Our Future
NZ Psychological Society: Remembering The Past Guides Our Future  New Zealand Olympic Committee: Motherhood In Focus For Wāhine Toa Graduates Ahead Of Mother's Day
New Zealand Olympic Committee: Motherhood In Focus For Wāhine Toa Graduates Ahead Of Mother's Day