Specialist sign-off for cannabis would strain health sector
Specialist sign-off for cannabis would strain health sector
An independent survey of over 700 healthcare professionals reveals genuine concern that New Zealand’s health sector would struggle to cope if ‘specialist sign-off’ is required before a GP can prescribe medicinal cannabis.
Public consultation closes in less than a week on the Ministry of Health’s discussion document for New Zealand’s Medicinal Cannabis Scheme. Its recommendation for specialist sign-off has been widely condemned by the Royal New Zealand College of General Practitioners (RNZCGP), many medical experts, as well as patient advocates.
The country’s largest licensed medicinal cannabis company, Helius Therapeutics, commissioned Horizon Research to survey healthcare professionals last month. A majority of the 728 respondents were GPs, specialist consultants, junior doctors and nurse practitioners.
Since the discussion document was released on 10 July, it marks the only comprehensive survey on the views of New Zealand’s healthcare professionals on how medicinal cannabis should be prescribed and the potential impact on the health sector.
Executive Director of Helius Therapeutics, Paul Manning, says “the results confirm a growing fear that the country’s health system would struggle to cope, both in terms of the numbers of specialists available and the sheer number of referrals that would be created.”
On the issue of capacity, 71% of all survey respondents said there would be not be enough specialists to cope with patients requiring approval for medicinal cannabis prescriptions; 15% thought there would be; and 14% were unsure. Among just GPs, 74% believed there would not be enough specialists.
On whether their practice or organisation would be able to cope with the likely demand created by referrals to specialists, 73% of all respondents said their workplace would not be able to meet demand or were unsure; while just 27% thought they would cope. When it came to ‘Physician - Specialist/Consultants’, 79% said their workplace would not be able to meet demand or were unsure; while 21% would cope.
Mr Manning says it’s also important to note that only 13% of those working in a public hospital or public clinic thought their workplace would be able to meet the extra demand created by referrals by specialists. Patients relying on the public health system will be disproportionately affected by access restrictions.
“Overwhelmingly, feedback from both doctors and specialists confirms the strong belief that GPs are already specialists in the field of general medicine, they know their patients best, and are perfectly capable of prescribing cannabis-based products on their own, just as they do with other prescription medicines.”
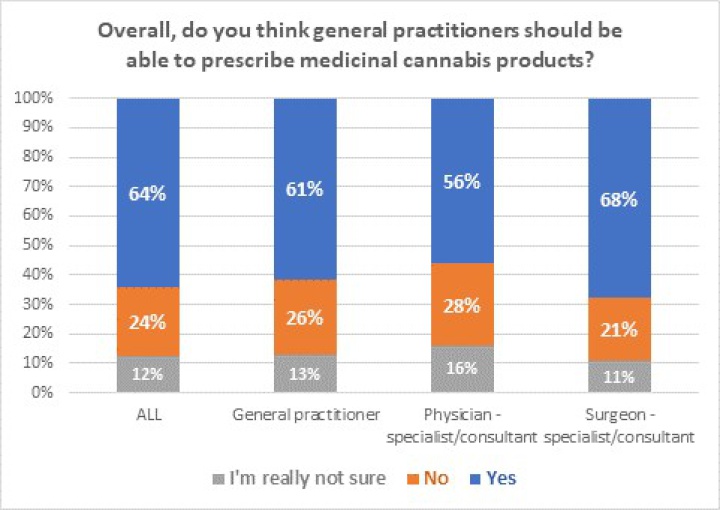
Nearly two-thirds, or 64%, of all respondents believe GPs should be empowered to prescribe medicinal cannabis products; 24% disagree; and 12% are unsure. When ‘Surgeon – Specialist/Consultants’ were asked, that rose to 68%; with 21% disagreeing; and 11% unsure.
International experience, and research by Helius, shows that New Zealand doctors can expect to be flooded with enquiries regarding medicinal cannabis for chronic pain. After all, it’s the number one condition that patients seek medicinal cannabis for, and it’s the leading condition that doctors are most likely to prescribe medicinal cannabis for.
“We’d quickly reach crisis point, as there are simply not enough pain specialists practicing in New Zealand to deal with what would be an unprecedented number of chronic pain referrals from GPs. Serious concerns about the lack of capacity in our healthcare system to cope have now been confirmed by the very people who work within it. This is a real wake-up call.”
Mr Manning says the extent of the public groundswell for medicinal cannabis was captured in an independent survey of 1,100 New Zealanders, released by Helius in May. The results showed that 14% of respondents ‘definitely’ plan on accessing medicinal cannabis products once they become more widely and legally available next year, equating to a staggering 431,900 New Zealanders.
Since the discussion document was released last month, patient advocates have also raised concerns over access to medicinal cannabis being impeded. This is a concern that most healthcare professionals share, according to the latest Horizon study.
A clear majority of respondents, 58%, believe there would likely be delays in patient access to medicinal cannabis products if prescriptions need to be signed off by a specialist. Over a third, or 37%, are concerned that the cost to many patients would become too great, while just 13% of all respondents agreed with the statement that ‘specialist sign-off would not reduce access to medicinal cannabis products’.
Mr Manning says the survey of senior healthcare professionals reaffirms New Zealanders’ strong desire for medicinal cannabis to be made widely accessible for the hundreds of thousands of patients who stand to benefit from its therapeutic potential.
“It’s now clear both anecdotally and statistically, that if New Zealand’s Medicinal Cannabis Scheme is to be effective it needs to entrust our highly-valued GPs with the professional discretion to prescribe medicinal cannabis to their patients.
“Helius believes every New Zealander has a natural right to a pain-free existence. Our Government and Health Minister are also clearly driven by improved patient access to medicinal cannabis products. Let’s now collectively ensure we have a scheme in place that will deliver for Kiwis from day one,” says Paul Manning.
The public has until 5.00pm on Wednesday, 7 August to submit feedback on the Ministry of Health’s discussion document on the proposed regulations.
Commissioned by Helius Therapeutics and carried out independently by Horizon Research, the results are from a nationwide survey of 728 healthcare professionals in New Zealand, conducted by Horizon Research between 17 and 22 July 2019. At a 95% confidence level, the maximum margin of error on the overall sample is ± 3.7%.
Key results:


 Gordon Campbell: On The Political Panic Over Immigration
Gordon Campbell: On The Political Panic Over Immigration Greenpeace: New Climate Report Yet More Reason To Reduce Dairy Herd
Greenpeace: New Climate Report Yet More Reason To Reduce Dairy Herd Better Public Media: Opposing Plans To Scrap The BSA
Better Public Media: Opposing Plans To Scrap The BSA Internal Affairs: Citizenship Test For Citizenship By Grant Applicants From Late 2027
Internal Affairs: Citizenship Test For Citizenship By Grant Applicants From Late 2027 Dayenu: Condemning Use Of Government Funding For Extremist Report On Antisemitism
Dayenu: Condemning Use Of Government Funding For Extremist Report On Antisemitism PSA: Councils Must Work With Unions And Communities In Fast-Track Reform
PSA: Councils Must Work With Unions And Communities In Fast-Track Reform Tauranga City Council: Mauao Restoration Work Has Begun
Tauranga City Council: Mauao Restoration Work Has Begun


